Last updated on
Take control of your slipped disc discomfort because our comprehensive blog post provides crucial insights on effective treatments, exercises, and preventative measures.
Key takeaways:
- Slipped disc is when gel pushes through a tear.
- Spine consists of vertebrae, discs, nerves, and tissues.
- Aging, trauma, poor posture can cause slipped disc.
- Symptoms include pain, numbness, weakness, and more.
- Treatments include medication, therapy, surgery, and prevention.
Table of Contents
Understanding a Slipped Disc
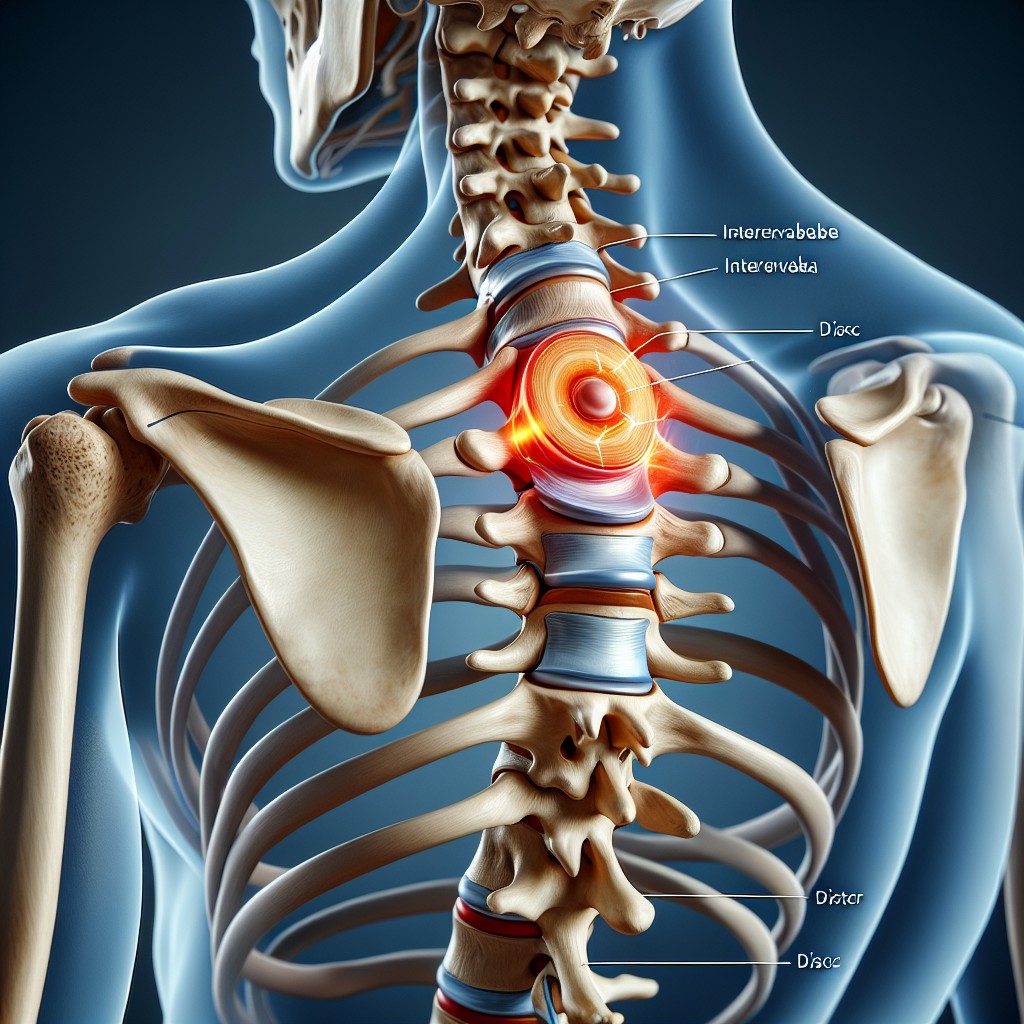
The spine is a complex structure, consisting of vertebrae, discs, nerves, and other tissues, working together to support your body and enable movement.
A slipped disc occurs when the soft inner gel of an intervertebral disc pushes through a tear in the disc’s tougher exterior.
This herniation can press on surrounding nerves and cause pain or discomfort.
Different terms, such as herniated, ruptured, or prolapsed disc, are often used interchangeably to describe this condition.
The severity and symptoms can vary widely, but understanding that a slipped disc is essentially a structural issue with one of the spine’s shock absorbers is the first step towards addressing it.
Anatomy of the Spine
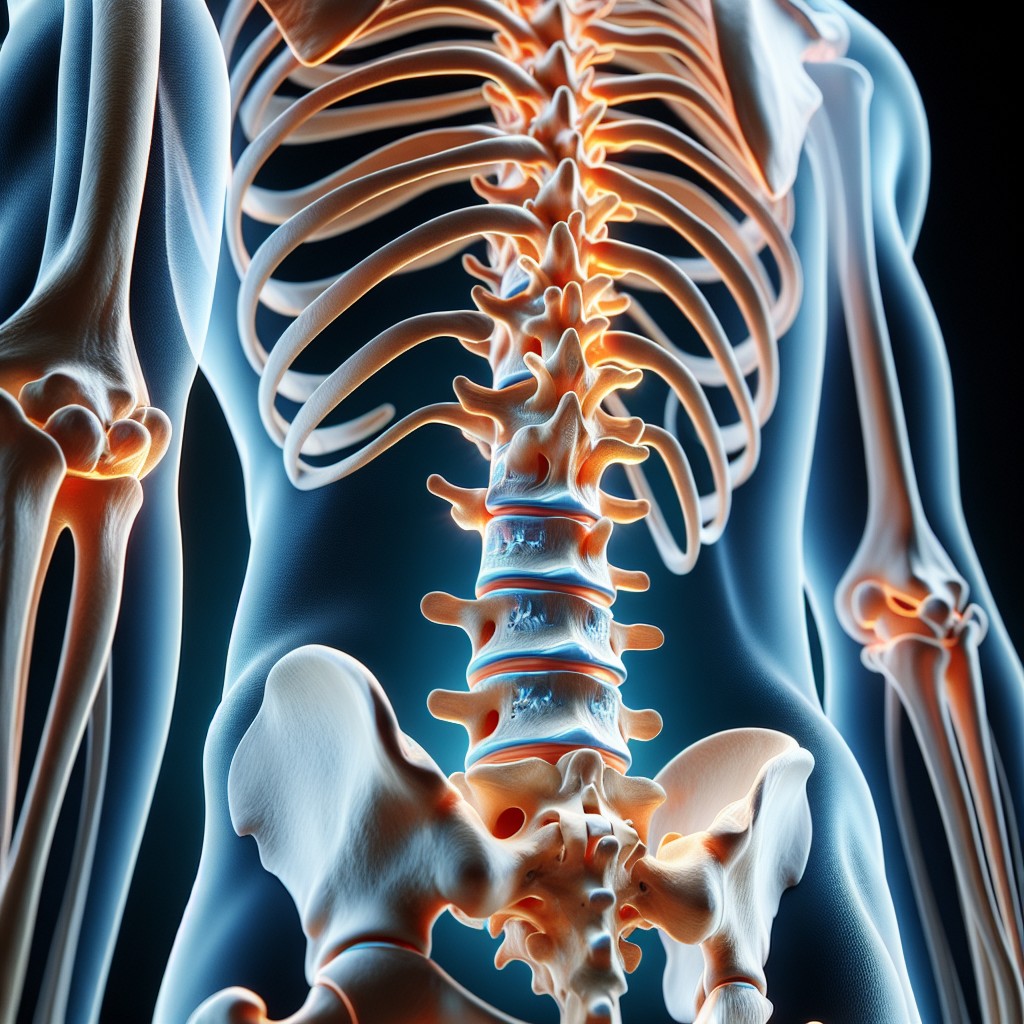
The spine, also known as the vertebral column or backbone, is a complex structure that provides the body with both support and flexibility. Let’s simplify its anatomy:
- Vertebrae: The spine consists of 33 individual bones stacked one on top of the other, divided into regions that include the cervical (neck), thoracic (upper back), lumbar (lower back), sacral, and coccygeal (tailbone) areas.
- Intervertebral Discs: Each vertebra is separated by cushions known as intervertebral discs. These discs have a tough outer layer called the annulus fibrosus and a gel-like center, the nucleus pulposus, which helps absorb shock and maintain spinal flexibility.
- Nerves: The spinal cord runs through a canal in the center of this vertebral column, from which spinal nerves emerge at each level, connecting the brain to various parts of the body.
- Supporting Structures: Ligaments, tendons, and muscles are integral to the spine’s function, providing support and allowing for movement while also protecting the spinal cord and nerves.
Understanding the spine’s basic structure is crucial in recognizing how a slipped disc can create discomfort and disrupt this well-engineered system’s function.
Causes of a Slipped Disc
A range of factors can lead to the development of this condition:
- Aging is a primary factor, as discs naturally lose their flexibility and fluid content over time, making them more susceptible to tearing or rupturing.
- Repetitive movements or overuse, especially in occupations or sports requiring constant back motion or heavy lifting, increase the risk.
- Trauma from falls, accidents, or sudden movements can cause immediate disc damage.
- Poor posture strains spinal alignment, putting excess pressure on the disc.
- Obesity adds extra weight and stress to the discs in the lower back.
- Smoking inhibits nutrient delivery to the discs, contributing to their degeneration.
- Genetic disposition may also play a role, as disc problems can run in families.
Symptoms of a Slipped Disc
Identifying symptoms early is key in managing a slipped disc. Pain is the most common indicator, often manifesting as a sharp or burning sensation in the back. This discomfort can radiate, moving to the buttocks, thigh, calf, and even extending to the foot.
Numbness or tingling in the affected area is another red flag. These sensations can indicate nerve irritation or damage from the protruding disc material.
Weakness is a symptom that can disrupt daily activities. The muscles served by the affected nerves might weaken, affecting your ability to hold items or causing stumbling while walking.
Some individuals may experience symptoms on one side of the body, depending on the location of the slipped disc. The severity of the symptoms can vary, from mild discomfort to debilitating pain, and activities like sitting, bending, or sneezing may exacerbate them.
Understanding these signs is crucial for seeking timely medical attention and preventing further complications.
Diagnosis of a Slipped Disc
Diagnosing this condition starts with a thorough medical history and physical examination. Your doctor will ask about your symptoms and any recent activities that may have led to back pain. During the physical exam, they might check for areas of tenderness, the range of motion of your spine, and any signs of nerve irritation or muscle weakness.
If your symptoms and physical exam suggest a slipped disc, your doctor might recommend imaging tests for a clearer picture. An MRI scan is the most common test, providing detailed images of the spine’s bones and soft tissues, including the discs. CT scans and X-rays, though less commonly used for discs, can also help rule out other conditions that might cause similar symptoms.
In some cases, your doctor might also conduct nerve studies. Electromyography (EMG) and nerve conduction velocity (NCV) tests assess the electrical activity in your nerves, helping to pinpoint the affected area and the degree of nerve damage.
Remember, early and accurate diagnosis is key to effective treatment and recovery, so be sure to consult with your healthcare provider if you suspect a slipped disc.
Treatment Options for a Slipped Disc
Several treatment approaches can help alleviate the discomfort caused by a slipped disc and promote healing. Initially, conservative treatments are often recommended, including:
- Medication: Over-the-counter pain relievers such as ibuprofen or acetaminophen can reduce inflammation and pain. In more severe cases, doctors may prescribe muscle relaxants or stronger painkillers.
- Physical Therapy: A therapist can demonstrate stretches and exercises tailored to strengthen the back and abdominal muscles, thereby supporting spinal health and relieving pressure on the herniated disc.
- Heat and Cold Therapy: Applying heat can encourage blood flow and soothe tense muscles. Cold packs, alternatively, can reduce swelling and numb the affected area, offering temporary pain relief.
- Epidural Injections: Corticosteroids injected into the epidural space can suppress inflammation around the nerve roots, providing significant pain relief for some individuals.
- Chiropractic Care: Licensed chiropractors may use spinal manipulation to reduce disc herniation, improving mobility and decreasing pain.
If conservative treatments do not provide relief after several weeks or months, surgical options might be considered:
- Microdiscectomy: A minimally invasive surgery where only the portion of the disc pressing on the nerve is removed.
- Laminectomy: Involves the removal of part of the bone overlying the spinal canal to relieve nerve pressure.
- Artificial Disc Replacement: Reserved for certain cases, it involves replacing the damaged disc with a synthetic one.
Remember, the right treatment depends on the specifics of the condition and individual patient needs. Consulting with healthcare professionals is crucial to determine the most appropriate course of action.
Preventing Slipped Discs
Maintaining a strong and flexible spine is key to avoiding disc-related injuries. Here are actionable strategies to help prevent the onset of a slipped disc:
- Regular Exercise: Incorporate a balanced regime, including core strengthening, flexibility, and cardiovascular workouts, to support spinal health.
- Proper Lifting Techniques: Always lift objects with your legs, not your back, and avoid twisting your spine while carrying heavy loads.
- Ergonomic Posture: Be conscious of your posture when sitting, standing, or walking. Use ergonomic chairs and take frequent breaks if your job requires long hours at a desk.
- Healthy Weight: Keeping within a healthy weight range reduces the load and stress on the spine.
- Stay Hydrated: Adequate hydration helps maintain the elasticity and height of intervertebral discs.
- Quit Smoking: Smoking decreases oxygen supply to the discs, making them more prone to degeneration.
Incorporating these habits into your daily routine can significantly lower the risk of disc slippage and foster overall spinal health.
Managing Pain From a Slipped Disc
Dealing with the discomfort caused by a slipped disc starts with conservative methods:
- Rest: Initially, limiting activities that exacerbate pain is crucial. However, prolonged inactivity can lead to muscle weakness, so transition to gentle movement as recommended.
- Heat and Cold Therapy: Applying heat can relax tight muscles while cold packs reduce inflammation and numb the sore area.
- Over-the-Counter Medications: Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen can relieve pain and reduce inflammation.
- Physical Therapy: Tailored exercises can strengthen back muscles and support the spine, improving flexibility and reducing pressure on the affected disc.
- Stretching: Gentle stretches can help maintain mobility and reduce tension in the muscles surrounding the spine.
- Proper Posture: Adopting an ergonomic work environment and being mindful of posture can help to reduce the strain on your spine.
Consult with a healthcare provider before starting any new pain management regime to ensure it aligns with your specific health needs.
When to See a Doctor
If you experience any of the following, it’s time to consult a healthcare professional:
- Persistent or intensifying back pain that hinders daily activities
- Numbness or tingling sensations in your arms or legs
- Decreased strength or coordination, particularly in the limbs
- Loss of bowel or bladder control, which can indicate a more severe condition known as cauda equina syndrome
Early intervention can improve your chances for a speedy and full recovery. A doctor can provide a proper diagnosis and recommend a suitable treatment plan tailored to your condition. Remember, listening to your body is key; do not hesitate to seek medical advice if your symptoms are causing concern.
Success Stories: Overcoming a Slipped Disc
Many individuals have navigated the journey from a slipped disc to full mobility with great success. Hearing about others overcoming the pain and limitations can be a source of motivation and hope.
- Physical Therapy Triumphs: Tailored exercises have enabled patients to strengthen the muscles supporting their spine, which is pivotal in the recovery and prevention of future issues.
- Surgical Success: While often considered a last resort, some individuals find that after surgical intervention, their symptoms are significantly reduced or even eliminated, allowing them to return to activities they love.
- Holistic Approaches: Incorporating yoga and Pilates to improve flexibility and core strength has been life-changing for many, highlighting the importance of a holistic approach to spinal health.
- Discipline in Daily Routines: Simple lifestyle changes, such as maintaining proper posture and incorporating ergonomic furniture, have proven effective for countless individuals in mitigating symptoms.
- Pain Management Prowess: Mastering pain management through techniques like hot/cold therapy, acupuncture, or chiropractic care has provided essential relief during recovery phases.
Reading about these affirming stories serves as a testament to the resiliency of the human body and the array of tools available to aid in the recovery from a slipped disc.




